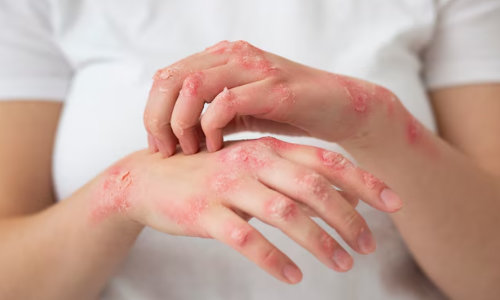
Ringworm – Causes, Symptoms, Treatment
Ringworm, a fungal infection, manifests as a circular rash on the skin. Although conditions such as eczema and psoriasis may mimic ringworm, distinct variations exist in their appearance and treatment approaches. Ringworm treatment is one of the specialities of Dr Monga’s in Delhi. If you are also suffering from the condition, book a consultation today and get rid of the irritating infection.
What is Ringworm?
It may come as a surprise to you, but ringworm is caused by a fungus, not a worm. This common and contagious skin infection earns its name from the circular, itchy skin lesion, resembling a ring, which can be scaly. It spreads readily through close contact.
Ringworm is contracted through contact with an infected person, animal, or object. Depending on the affected body part, ringworm goes by different names. When it affects the body, it is called tinea corporis, impacting the arms, legs, torso, and face. Treatment for ringworm involves antifungal medication, which is available over the counter or through a prescription.
How do I know if I have ringworm?
Ringworm manifests initially as discolored patches, often with scales, on the affected areas. These patches typically present as red on lighter skin tones or brown-gray on darker skin tones.
Symptoms can vary depending on the location of the infection. For a skin infection, you may experience the following:
- Recurrent itchiness
- Itchy or scaly patches that are red, brown, or gray, or raised areas of skin called plaques
- A round, flat patch of itchy skin
- Patches that develop blisters or pustules
- Patches that resemble a ring with deeper color on the outside
- Patches with edges that are defined and raised
- Overlapping rings
- Hair loss
Symptoms by type
The appearance of ringworm may vary depending on which body part it has infected. Doctors use different terminologies for ringworm depending on which body part it appears on.
- Ringworm of the body: This type of ringworm is known as tinea corporis. It often appears on your torso or limbs in the form of patches and characteristic round ring shape.
- Ringworm of the scalp: This type of ringworm is known as tinea capitis. It typically begins with localized scaling on the scalp, which progresses to itchy, scaly bald patches. It primarily affects children. Hair surrounding the impacted region might become brittle or shed, resulting in the formation of bald spots.
- Ringworm of the beard: Beard ringworm, known as Tinea barbae, impacts the cheeks, chin, and upper neck, potentially resulting in patches of hair loss. Its appearance can resemble acne, folliculitis, or other skin conditions. Some individuals may also experience fatigue or swollen lymph nodes.
- Ringworm of the hand: Hand ringworm, or Tinea manuum, typically arises from contact with another infected area, such as the groin or foot. Hand infection may manifest as extremely dry skin with deep cracks on the palm. If the infection spreads, ring-shaped patches may appear on the back of the hand.
- Jock itch: Jock itch, referred to as Tinea cruris, is a ringworm infection affecting the skin around the groin, inner thighs, and buttocks. It predominantly affects men and adolescent boys. Initially presenting as an itchy red, brown, or gray rash where the leg and body meet, the itching may exacerbate post-exercise and may not respond to anti-itch creams like steroid creams, which could potentially worsen the rash.
- Athlete’s foot: Athlete’s foot, or Tinea pedis, is a ringworm infection of the foot, commonly observed in individuals who frequent public areas barefoot, such as locker rooms, showers, and swimming pools. It typically begins as dry, scaly skin between the toes, potentially spreading to the sole and heel, accompanied by symptoms like itching, stinging, burning, blistering, or peeling skin, often accompanied by an unpleasant odor.
- Tinea unguium: Tinea unguium, a fungal ringworm infection of the nails, more frequently affects toenails due to the moist, warm environment provided by footwear. Affected nails may thicken or change color, possibly becoming cracked or detached from the nail bed.
Symptoms by stage
Ringworm may not become visible immediately upon initial exposure to the fungus. It could take up to 3 weeks before symptoms begin to manifest. The progression of the infection may unfold through the following stages:
- Initial stage: At this point, you might observe a discolored, irritated patch of skin. Sometimes, it may appear dry and scaly, lacking the typical ringworm appearance.
- Second stage: During this phase, the lesion tends to increase in size. The center of the rash may resemble healthy skin, surrounded by a scaly area.
Prompt initiation of treatment upon noticing the initial signs of a ringworm infection is crucial. Failure to do so could result in its spread and exacerbation.
Causes of Ringworm Infection
Ringworm, a contagious fungal infection, stems from common mold-like parasites dwelling on the cells of the outer skin layer. It spreads through various means:
- Human to human: Ringworm generally transmits via direct skin-to-skin contact with an infected individual.
- Animal to human: You can contract ringworm infection by touching an animal carrying the infection, often happening during petting or grooming sessions with dogs or cats. It is also relatively common in cows.
- Object to human: Ringworm can potentially spread through contact with objects or surfaces recently touched or rubbed by an infected person or animal, including clothing, towels, bedding, linens, combs, and brushes.
- Soil to human: In rare instances, ringworm may transfer to humans through contact with contaminated soil. Infection is more likely with prolonged exposure to highly infected soil.
Risk factors
Your likelihood of developing ringworm of the body increases if you:
- Reside in a warm climate
- Maintain close contact with an infected individual or animal
- Share clothing, bedding, or towels with someone afflicted by a fungal infection
- Engage in sports involving skin-to-skin contact, like wrestling
- Wear tight or constrictive clothing
- Possess a weakened immune system
How is ringworm diagnosed?
Your healthcare provider can diagnose ringworm by examining your skin and evaluating your symptoms. They may also scrape the affected area to analyze the skin cells under a microscope. Typically, the presence of scales confirms the diagnosis of ringworm.
Ringworm Treatment
Numerous over-the-counter and prescription antifungal medications are quite popular for ringworm infection treatment. These ringworm medications are available in various forms, such as creams, gels, or powders. In cases of more extensive ringworm, your healthcare provider may opt for oral antifungal medication for treatment.
Antifungal creams and powders
Over-the-counter (OTC) antifungal creams, gels, or powders often provide effective relief.
Should your symptoms worsen or fail to improve after two weeks, consulting your healthcare provider may be necessary for a prescription oral ringworm medication.
Oral medication
If you have ringworm on your scalp or widespread on your body, your healthcare provider might prescribe oral antifungal medication. Typically, these medications are prescribed for durations ranging from one to three months.
Antifungal shampoo
Antifungal shampoo can help prevent the spread of scalp ringworm. While it may not cure the infection, it can aid in controlling its spread. It, however, is typically necessary to complement shampoo use with prescribed oral antifungal medication for effective treatment. Additionally, unaffected family members may benefit from using the shampoo as a preventative measure.
Home remedies for ringworm
Home remedies such as apple cider vinegar or tea tree oil are generally ineffective in treating ringworm. Apple cider vinegar may even lead to open sores or inflammation. While tea tree oil possesses antifungal and antimicrobial properties, its efficacy in treating ringworm is not well-established.
Additionally, it is important to treat your home environment as well, as the ringworm fungus can linger on surfaces for months. Disinfectant sprays or bleach can effectively eliminate the fungus. Washing clothes, sheets, and towels in hot water with detergent is also essential to prevent the spread of ringworm.
Steroid creams
Corticosteroid creams may aid in reducing inflammation, but they should not be used to treat ringworm. In fact, their use may exacerbate the infection.
Starting ringworm treatment on your own without getting the severity evaluated by a professional healthcare provider may not only prolong the recovery period but also worsen the symptoms. Hence, it is advised to see a healthcare practitioner to get the best possible care and quick recovery.
Dr Monga’s in Delhi has multiple doctors who are very apt in ringworm treatment, and have treated thousands of patients over the years. If you are also facing any symptoms of ringworm infection, you should immediately book an appointment with Dr Monga’s in Delhi.
What cures ringworm?
Mild cases of ringworm typically resolve within a few weeks, while more severe infections may necessitate treatment for six to 12 weeks.
Additionally, here are some measures to promote healing:
- Keep the affected area clean and dry.
- Apply antifungal lotions, creams, or ointments consistently throughout the entire treatment period.
- Avoid touching the affected area and ensure you wash your hands thoroughly before touching other parts of your body.
Will ringworm go away on its own?
Ringworm may resolve spontaneously without treatment, especially in milder cases, but this process typically takes longer compared to treatment.
The duration of contagion for ringworm can vary depending on factors such as the individual’s immune system, the severity of the infection, and the effectiveness of any treatment undertaken. It is important to note that even after symptoms have subsided, the fungus may still be contagious until it is completely eradicated from the affected area.
Therefore, it is advisable to consult with a healthcare provider for proper diagnosis and treatment to minimize the risk of spreading the infection and to ensure complete resolution.
Prevention
Trying to prevent ringworm can be tricky but with proper understanding of how the fungus spreads, you can save yourself from getting infected to a large extent.
How can I prevent ringworm?
Ringworm thrives in damp, warm environments, and the fungus can persist on various surfaces for months. Preventing ringworm involves adopting the following practices:
- Change your socks and underwear daily, or more frequently if they become damp or soiled.
- Shower immediately after participating in contact sports or exercising.
- Wear sandals or shower shoes in public areas like pools, locker rooms, and showers.
- Ensure thorough drying of your skin after showering, especially between your toes.
- Refrain from sharing towels, washcloths, sheets, clothes, combs, or other personal items related to hygiene.
- Wash your clothes, athletic gear, sheets, and towels in hot water with detergent.
- Disinfect surfaces using bleach or sprays.
- Treat pets for ringworm if they are infected.
- Wash your hands thoroughly after contact with animals.
Factors such as having a weakened immune system or living in a damp, warm climate can heighten the risk of fungal infections.
Can ringworm come back?
Indeed, ringworm has the potential to recur. However, with proper treatment adherence, it can be effectively eradicated. It is crucial to follow your healthcare provider’s treatment plan diligently until the infection is completely cleared. Discontinuing treatment prematurely or failing to adhere to the prescribed regimen may result in the recurrence of infection.
What are the complications of ringworm?
If you suspect that you or your child has ringworm, avoid using anti-itch creams containing corticosteroids. These creams can compromise your skin’s natural defenses, potentially leading to the spread of the infection and affecting larger areas of the skin. In rare instances, the ringworm fungus may penetrate deeper into the skin, complicating treatment.
Scalp ringworm can result in a painful condition known as kerion, characterized by the development of crusty, pus-filled sores, often accompanied by hair loss and scarring.
Living With Ringworm
Living with ringworm can be challenging, but with proper management and treatment, it is possible to effectively control the infection and prevent its spread.
When should I call the doctor?
Contact your healthcare provider promptly if you experience any of the following concerning situations related to a ringworm infection:
- Appears on your scalp
- Exhibits signs of infection, such as redness and swelling
- Occurs during pregnancy
- Spreads to other areas of your body
- Does not show improvement after using over-the-counter antifungal medication as directed.
Seeking medical advice in these scenarios ensures proper evaluation and management of the infection, especially in cases requiring specialized treatment or during specific medical conditions like pregnancy.
What questions should I ask my doctor?
If you or your child develop ringworm, you are most likely to have multiple queries to ask your healthcare provider. You may inquire about:
- How did I get ringworm?
- How long is ringworm contagious?
- Should I (or my child) stay home from work/school until the ringworm infection is gone?
- What steps can I take to prevent ringworm from spreading to other parts of my body?
- What steps can I take to prevent ringworm from spreading to other people?
- What is the best treatment for ringworm?
- Should I avoid any medications or treatments?
- What steps can I take to keep from getting ringworm again?
- How can I tell if my pet has ringworm?
- Should I look out for signs of complications?
FREQUENTLY ASKED QUESTIONS
If you experience pain or discomfort during any attempt at vaginal penetration, whether it be sexual intercourse, inserting a tampon, or during a gynecological exam, you might have vaginismus. Common symptoms include a burning or stinging sensation, tightening or clenching of the vaginal muscles, and anxiety about penetration. For a definitive diagnosis, it’s important to consult with a healthcare professional who can perform a thorough evaluation.
Vaginismus can be treated effectively, and many people experience significant improvement or complete resolution of their symptoms with the right treatment. This often involves a combination of physical therapy, psychological counseling, and sometimes medical treatments. The duration and success of treatment can vary from person to person, but with patience and persistence, relief is achievable.
To relax vaginal muscles, consider practicing deep breathing exercises, progressive muscle relaxation, and mindfulness meditation. Pelvic floor exercises, such as Kegel exercises, can also help you gain better control over these muscles. Using vaginal dilators and participating in pelvic floor physical therapy can further assist in learning to relax and control the vaginal muscles effectively.
When you perform a Kegel exercise, you are contracting the muscles of your pelvic floor. During sexual intercourse, your partner might be able to feel these contractions, which can sometimes enhance the sexual experience for both partners. Kegel exercises are beneficial for improving pelvic floor strength and control.
A strong pelvic floor typically means that you have good control over the pelvic muscles. Signs of a strong pelvic floor include the ability to start and stop the flow of urine easily, lack of urinary incontinence, and the ability to hold a contraction during a Kegel exercise for several seconds. If you are unsure about the strength of your pelvic floor, a pelvic floor physical therapist can perform an assessment and provide guidance.
- Diagnostic criteria for vaginismus (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6816375/)
- Effectiveness of treatment for vaginismus (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6816375/)
- Relaxation techniques for pelvic floor muscles (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5092612/)
- Understanding and Treatment of Vaginismus (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3682006/)
- Sensation during Kegel exercises (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4760628/)
- Assessing pelvic floor strength (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4639464/)